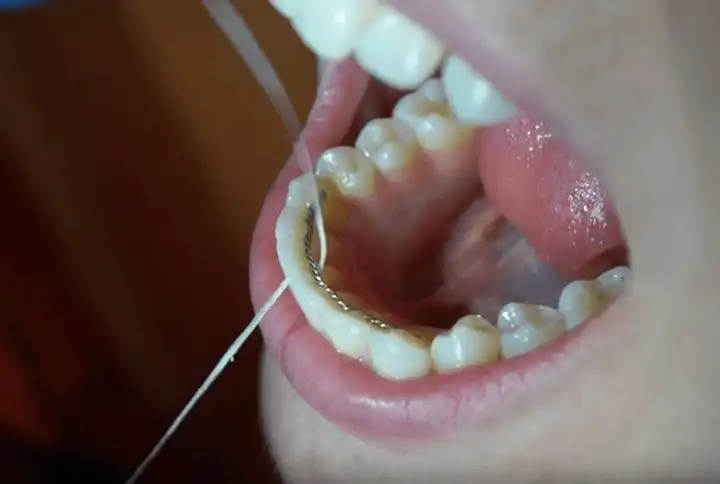
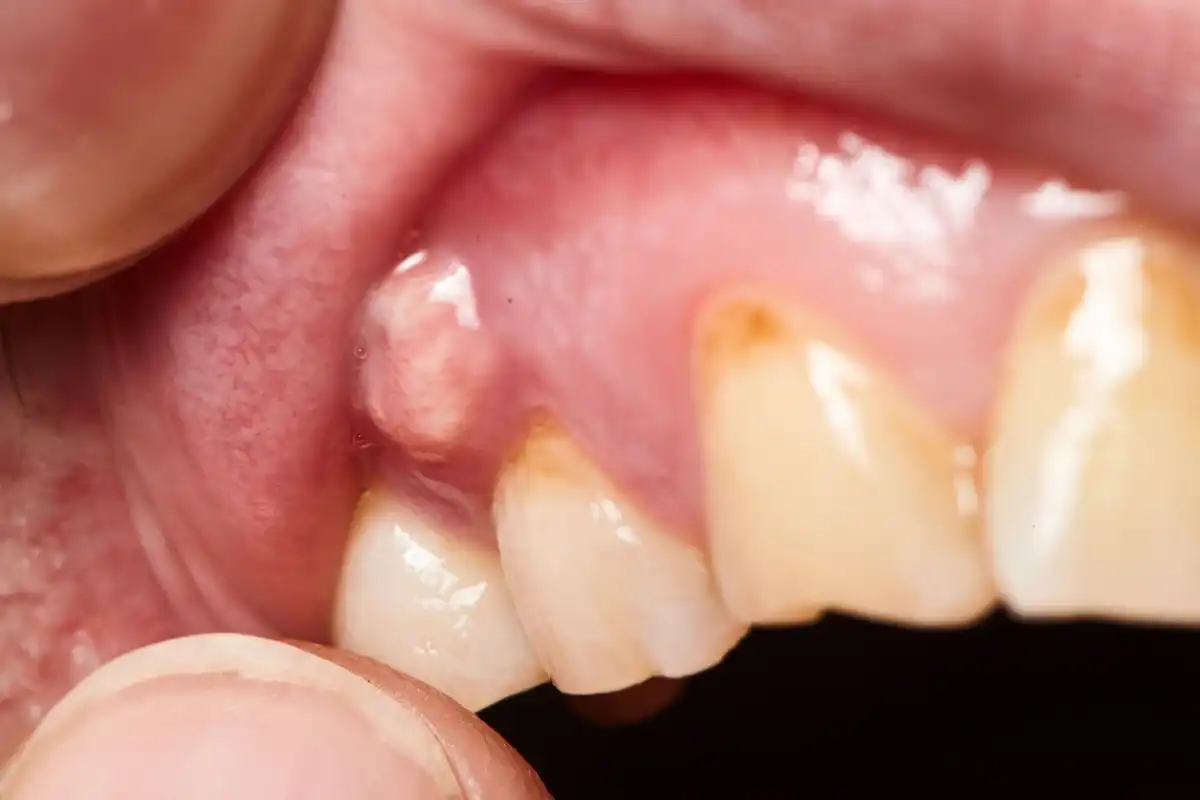
What Does Dry Socket Look Like Compared to a Blood Clot?

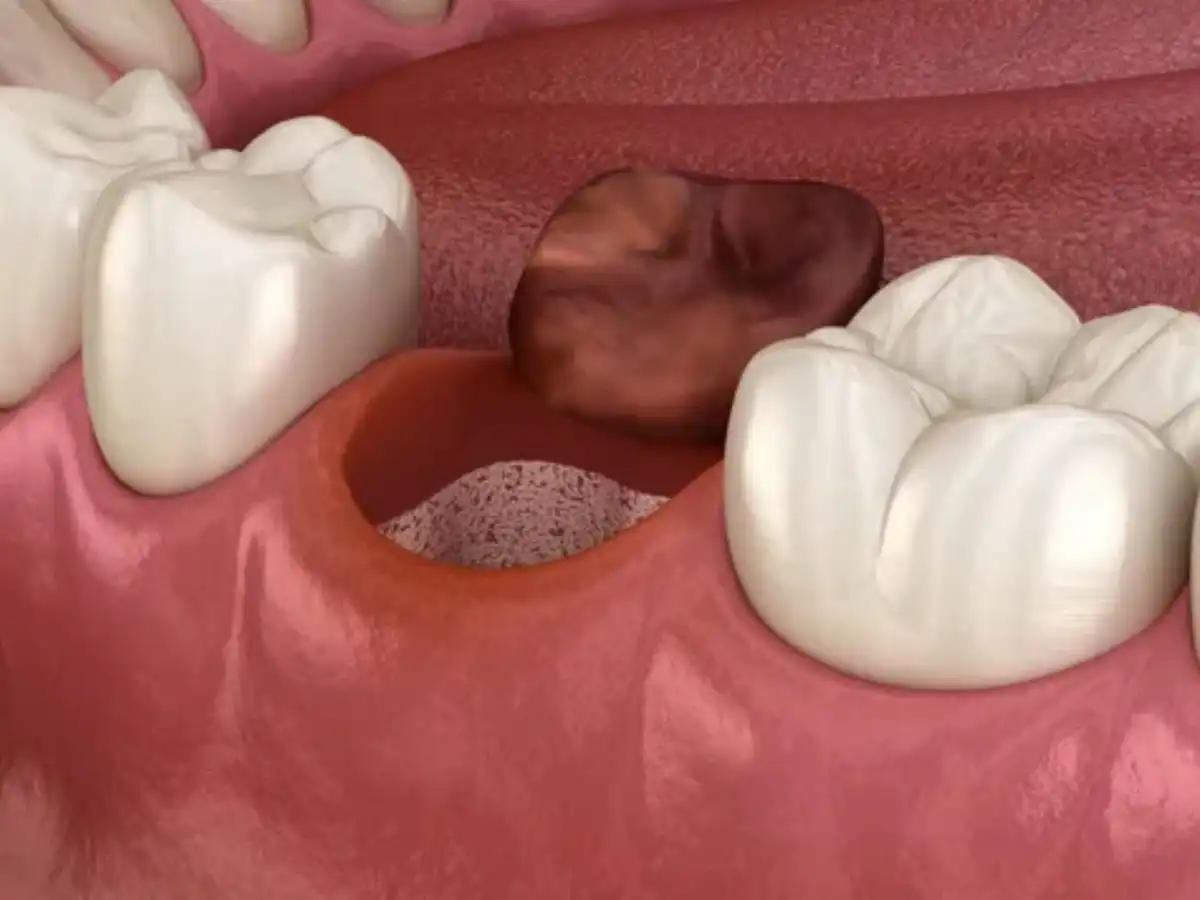
What Are Dry Socket Causes?
A dry socket is when the tooth extraction site — that is, the opening left in the bone after a tooth is taken out — doesn’t heal properly. Normally, you would have a blood clot form inside of the socket to protect the exposed bone and nerves. From there, the gums would grow back over it.
But with a dry socket, that blood clot either doesn’t form, or it’s disrupted. A dry socket in wisdom tooth cases will usually result in moderate to severe discomfort, lasting up to two weeks following the procedure.
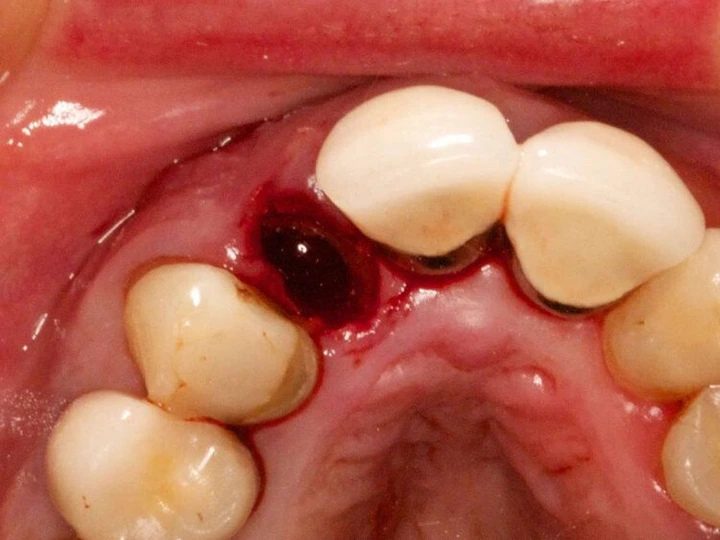
What does a dry socket look like? If you were to inspect it during a dental exam, it would be an open socket with visibly exposed bone and nerves.

Symptoms of Dry Socket
Generally speaking, the most common dry socket symptoms include pain and discomfort, along with a bad taste coming from that part of your mouth. You might not be able to eat because of how tender your mouth is.
Although you probably can’t see it, a tell-tale dry socket symptom is when there is visible bone at the tooth extraction site, signaling a lack of proper healing.
If you had a tooth pulled or recently completed a wisdom tooth extraction, you can usually expect any soreness or discomfort to improve within a couple of days of the appointment. But with a dry socket, you tend to experience increased pain a few days after the procedure. If your discomfort is noticeably worse when you should be feeling better, you probably have a dry socket.
What Do I Do If I Have A Dry Socket?
Although there are instances where someone just doesn’t heal well and still develops dry socket symptoms, many of the causes are due to inadequate “post-operative care.” In other words, you need to be following your dentist or oral surgeon's instructions on what you are or aren’t supposed to do after having a tooth pulled.
When you don’t abide by your post-operative instructions, you’re setting yourself up for common side effects like loosening of the blood clot, the clot never forming, or having it fall out altogether.
Here are some things you need to avoid to make sure you’re giving your body the best chance to heal.
1. Don’t Smoke Or Vape
Smoking dries out your mouth, making it more challenging to heal any type of sore, surgery, or infection. If you use tobacco products, try to take a break for a minimum of 2-3 days following your oral surgery.
2. Don’t Drink Through A Straw
There’s a theory that creating a vacuum by sucking through a straw could pull your blood clot out
3. Don’t Plan Heavy Exercise
Are you a long-distance runner? Weightlifter? Or an avid athlete of any sort? Take it easy for a few days. If you’re overexerting yourself, the blood pressure and increased heart rate can push your clot out from the inside.
4. Don’t Consume Alcohol, Carbonated Beverages, Or Eat Hard/Crunchy Foods
There’s an increased chance of dry socket symptoms when certain foods/beverages irritate the site of your oral surgery.
5. Don’t Rinse Really Hard
Your dentist or oral surgeon will probably tell you that gentle swishing and then letting the water slowly fall out of your mouth is enough for the first few days. If you’re swishing hard, it creates a suction that could dislodge your clot.
Why Do You Get Dry Sockets?
Sometimes it seems like you do everything right and still get a dry socket. Be sure to go over your medical history with your dentist or oral surgeon before the tooth extraction, so they can rule out any risk factors. For example, someone with hemophilia or anemia isn’t going to have the same type of blood clotting or bleeding levels as a person who is healthy.
Usually, dry sockets are preventable. So, if you want to make sure you aren’t in pain after a wisdom tooth extraction, follow your dentist’s instructions to a T.
What Do Dry Sockets Look Like
The first photo shows a dry socket compared to the blood clot that forms after the tooth extraction and is a normal part of the healing process.
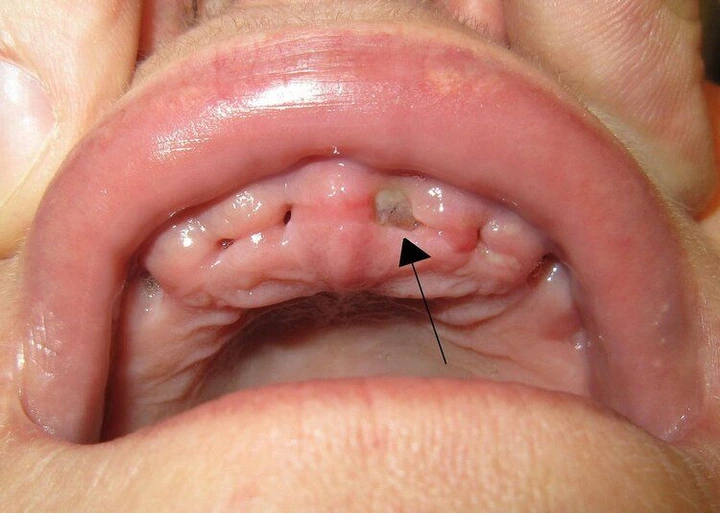
When To See A Dentist
The biggest complication from a dry socket is pain. If you feel worse 2-3 days after extraction or you have severe pain, you could have some type of infection or dry socket. At that point, you need to see your dentist. Your dentist or oral surgeon might even have you set up for a post-operative evaluation before you complete the tooth extraction. This appointment might seem silly, but it could help you avoid unnecessary complications.
How To Treat Dry Sockets
Dry socket treatment usually involves having your dentist flush out the socket and then placing a special medication or medicated dressing down into it. This artificial cover provides pain relief because there won’t be any outside stimuli or bacteria seeping into the area. From there, your body’s immune system can do the rest. You might have to see your dentist several days later to have the dressing removed. If there’s visible redness and swelling, you might also be given a prescription for an antibiotic.
Your dentist or oral surgeon will likely recommend taking an anti-inflammatory medication such as ibuprofen, not necessarily for the pain relief, but to reduce the amount of inflammation around your extraction site.
Quick Remedy
Gentle rinsing with warm saltwater can remove any food debris and reduce swelling while your mouth heals.
Prevention Of Dry Socket
Most people who get dry sockets are those who don’t follow their home care instructions. Although you might think that it won’t happen to you, there’s a reason why all of these guidelines are set in place.
Skipping a rule here or there may not cause a problem right then, because the symptoms might not show up until a few days later. At that point you may have broken the rule a few times, setting yourself up for some severe pain.
Dry Socket Recap
Dry sockets can happen in any extraction case, but most people associate them with wisdom tooth removal.
When most people start to feel better a couple of days after getting a tooth pulled, dry socket symptoms tend to peak 2-3 days after the procedure, making you feel worse.
The best way to avoid getting a dry socket is to follow your dentist’s home-care instructions, even if you think they’re not important. Don’t smoke. Don’t exercise. Don’t drink through a straw. Keep up with good oral health habits and don’t rinse your mouth out really hard.
A dry socket or alveolar osteitis happens when the blood clot in your extraction site comes loose or falls out. The only way to treat it and get out of pain is to see your dentist or oral surgeon as soon as any dry socket symptoms start to become evident. They’ll place a special medication down into the area to help you re-start the healing process.
Make your inbox smile!
Subscribe