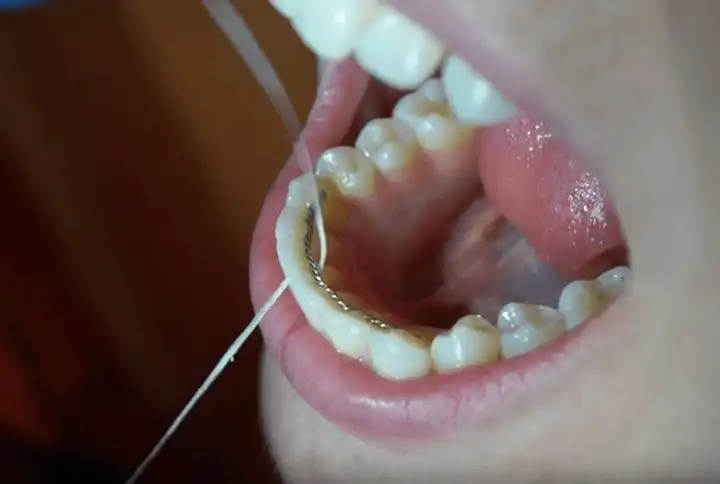
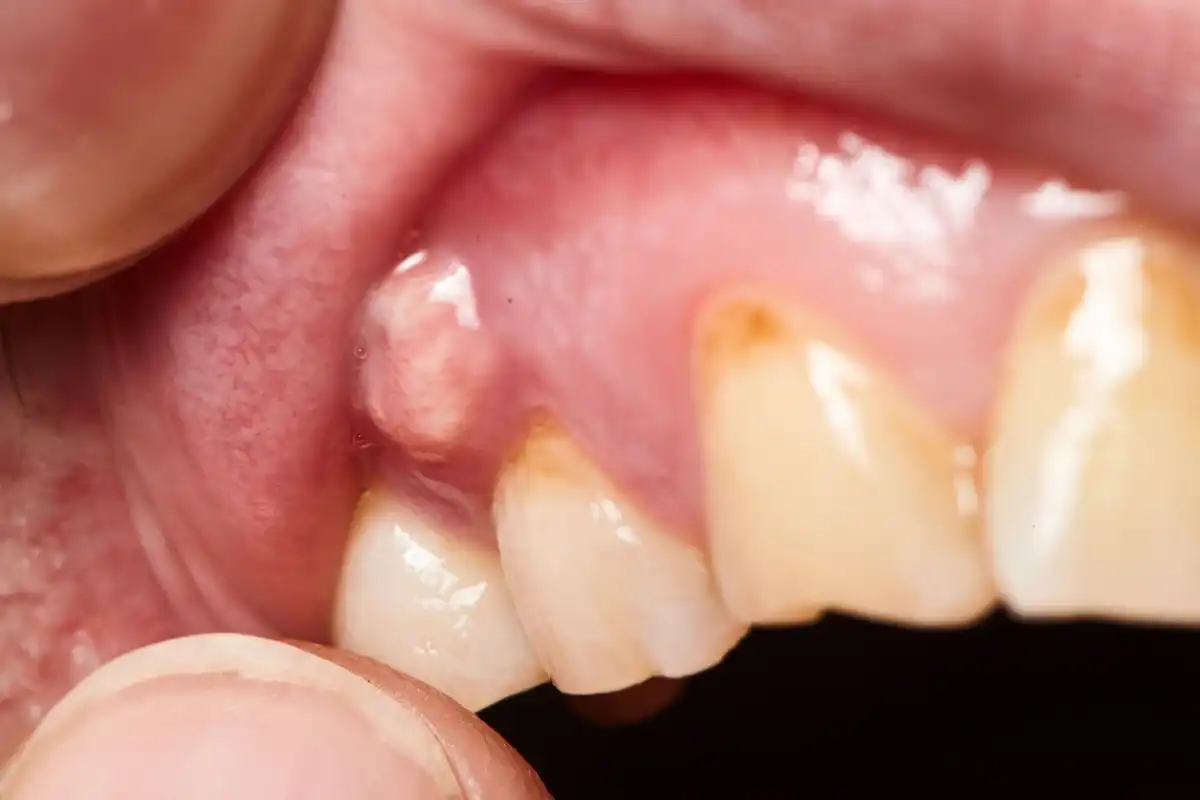
Pericoronitis: Swollen & Infected Wisdom Teeth

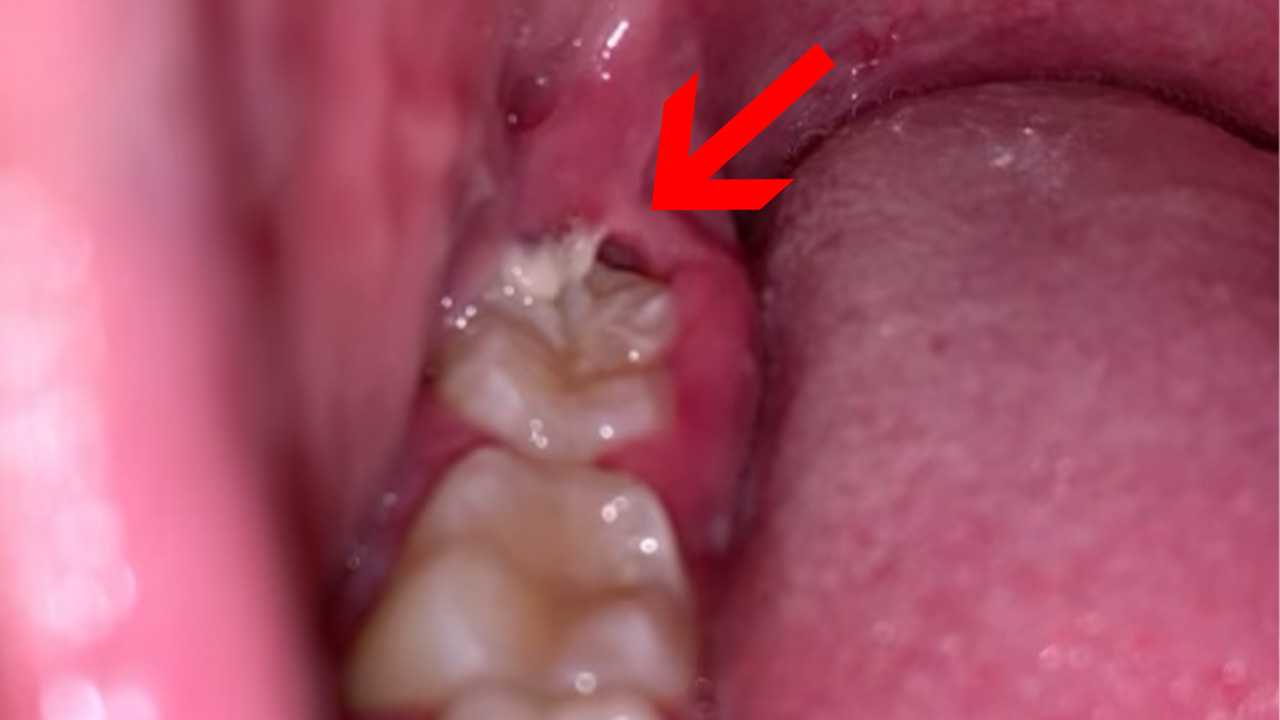
Pericoronitis is a condition that involves swollen gums around a wisdom tooth. Occasionally it can involve other teeth as well. The word “peri-“ means “around,” and “coron-“ in this situation is short for “coronal”, which is the crown of the tooth (the part you see above the gums.) And “-itis” means “inflammation of.” When you put them all together, you have inflammation around the crown of a wisdom tooth.
Acute pericoronitis infections can be extremely painful. And unfortunately, you can’t get rid of them on your own. You’ll need a dentist within a week or two to get to the source of your swollen gum and impacted wisdom tooth. In rare scenarios, pericoronitis is actually life-threatening.
What Is Pericoronitis?
Whenever your wisdom tooth starts to erupt, it “cuts” through your gum tissue (gingiva), just like all of your other teeth. But sometimes, the wisdom tooth only partially erupts because it’s wedged inside of the bone or against another tooth, making it partially impacted. As a result, the gums don’t pull all the way back from the chewing surface. You’re essentially left with a partially erupted tooth and a flap of gum tissue that’s still covering part of or the majority of your wisdom tooth. This flap over the erupting tooth is called the “operculum.”
In 95% of cases, pericoronitis involves the lower wisdom teeth because of the way they’re typically angled.
Is It Normal Pain Or Infected?
Teething pain affects wisdom teeth too! The only difference is it’s been years between cutting baby teeth and the soreness that comes from your third molars erupting. Most people notice some off-and-on discomfort, swelling, or aches coming from their wisdom teeth whenever they start to erupt.
But pericoronitis tends to be much more painful. The sharp ache may even make it impossible to chew in that area of your mouth. Plus, you can visibly see a swollen gum flap around or over the third molar.
What Causes Pericoronitis?
Pericoronitis is triggered by bacteria trapped under the gums, next to teeth. You could think of it like gingivitis on overdrive. When gingivitis evolves into periodontal (gum disease), it usually affects the roots of teeth. But in this case, the gums are still covering the crown of the wisdom tooth and infecting that area instead of the roots.

1. Impacted Wisdom Teeth
A partially impacted wisdom tooth will be only slightly visible above the gums. At least some portion of the crown is still covered by the gum tissue. Since there’s an opening in the gums, food and plaque will work their way down underneath it, around the tooth. Even if you’re brushing and flossing properly, you can’t remove those bacterial colonies.
Fully impacted teeth where the gums still fully cover the entire tooth don’t develop pericoronitis, but they can still be painful. This specific form of infection only occurs when some portion of the wisdom teeth are exposed within the oral cavity.
2. Trauma
As your wisdom tooth erupts and the gums over them stretch and pull back, you might accidentally bite down on the operculum (gum flap). When you do, it will likely become swollen, and you’ll keep suffering from repeated injuries in that area every time you eat.
Other common types of soft tissue trauma can come from eating “sharp” foods like tortilla chips. Or even accidentally slipping with your toothbrush and jabbing it into the gums.
3. Premature Tooth Loss
Teeth are programmed to fall out on a specific timeline. If you lose one prematurely for whatever reason, it can alter the normal tooth alignment patterns of other teeth. Long story short, it could cause the tooth below it to not fully erupt or come in crooked, which can lead to a gum flap over the crown. Normally your dentist or orthodontist can correct this scenario with early intervention.
4. Crowded Teeth
Crooked and crowded teeth are sometimes related to premature tooth loss because they shift and tilt out of alignment. Whenever they do, they can prohibit certain teeth from erupting all the way into the mouth, leaving an operculum/gum flap over specific teeth. Again, only about 5% of pericoronitis cases involve non-wisdom teeth, but it can happen!
5. Poor Oral Hygiene
There’s only so much you can do to clean around gum flaps on the erupting tooth. But if you have a syringe from your dentist, you can flush that area out with saltwater or mouth rinse. You can also improve your oral hygiene by using a water flosser to clean it each day. These steps are helpful as your tooth is erupting through the gums, but it might not be practical for long-term purposes. Good oral hygiene habits are always a must!
Symptoms of Pericoronitis
You’ll probably notice symptoms of pericoronitis resembling gingivitis or periodontal disease in the beginning. But since the inflammation covers the chewing surface of your tooth, you’re more likely to irritate it on an everyday basis. Severe swelling can gradually spread away from your tooth and into other areas of your face.
Acute Pericoronitis (short-term)
Acute pericoronitis usually last 3 to 4 days and symptoms associated with pericoronitis can include:
1. Infection Or Inflammation
Swollen gums around wisdom teeth are a dead giveaway for pericoronitis. Since infection causes tissues to swell up or become inflamed—like with gingivitis—you’ll notice a puffy layer of gums over at least a portion of the tooth. And more than likely, it will hurt whenever you bite down.
2. Pain or Discomfort
Pericoronitis is painful in and of itself. But it also can cause severe pain whenever you’re repeatedly biting down on the swollen tissue around your tooth. It may be impossible to avoid biting on it and irritating it due to the inflammation. More often than not, pericoronitis gradually becomes more painful as each day goes by, which is why it typically needs to be treated ASAP.
3. Red Gum Tissues
With the swelling around your tooth comes redness and possible bleeding. The red gums will stand out from the healthy pink gum tissue next to your other teeth, similar to if you had gingivitis elsewhere in your mouth.
4. Pus Around The Tooth
Severe gum infections can cause pus to weep from the area. This is why abscessed teeth frequently have fistulas or pimples on the gums next to those tooth roots. Only in this case the infection is draining out of the opening in your gums where the tooth has partially erupted. Most pus has a salty taste to it, and you may notice it coming and going.
5. Swelling In Your Face Or Neck
6. Difficulty Swallowing Or Breathing
If inflammation spreads into your face, neck or contributes to a respiratory infection, it can become life-threatening. Difficulty breathing may be noticeable due to the airway being restricted. At this point, emergency hospitalization is required.
Chronic Pericoronitis (long-term)
Chronic pericoronitis symptoms can be mild but keep recurring for months. Signs and symptoms of pericoronitis can include:
1. Bad Taste In The Mouth
As bacteria get trapped under your gum flap, they’ll start to multiply and produce smelly, gross byproducts as well as necrotic tissues. This can lead to a stinky situation that tastes just as bad as it potentially smells. You may notice a salty or sour taste from one specific area in your mouth.
2. Mild Discomfort & Inflammation
Mild discomfort whenever you bite down on the swollen tissue or inflammation around your tooth.
Treatment For Pericoronitis
The first step in treating any type of gum infection is first to address the source of the inflammation: bacteria. Your dentist will most likely use something like a syringe filled with a medicated mouth rinse to flush out any loose debris.
After the area is physically cleaned out, you will likely be prescribed an antibiotic. Take your medication as directed until the full course of the antibiotics are complete. This step will reduce inflammation and ease the pain. However, it will not prevent reinfection from occurring, given that the flap of tissue will continually harbor bacteria.
At this point, you usually have two options and they both depend on the placement and eruption pattern of your wisdom tooth. If your wisdom tooth is still erupting and expected to come into place—and it’s otherwise healthy—your dentist can use a soft tissue laser to remove the gum flap that’s covering the biting surface. This procedure is minimally invasive and requires little to no recovery time. An over-the-counter pain reliever is usually all that’s necessary.
Your other option is to have the wisdom tooth removed entirely. If your dentist doesn’t expect the partially erupted wisdom tooth to erupt properly, putting it at risk for recurring infections, the best thing to do is remove it for the sake of your overall oral health (and other teeth.)
How Common Is Pericoronitis?
People who have diabetes or a compromised immune system are more likely to get pericoronitis than their peers. However, conditions like mental health, stress, respiratory infections, and being on your period can also be to blame.
If the gum flap goes away as the tooth erupts, pericoronitis usually isn’t an issue. It’s only when the gum flap tends to continue covering the erupting wisdom teeth that you have to be on the lookout for infection. Especially if you’re biting on that area over and over, inducing trauma every time you eat.
Is Pericoronitis Only Involved With Wisdom Teeth?
95% of all pericoronitis cases are linked to the lower wisdom teeth. But that does not mean it’s impossible for them to occur elsewhere. In patients who have erupting molars (where flaps of gum tissue cover them at some point) but also struggle with crowding or partial impaction, a pericoronitis infection can still develop. These scenarios typically involve teeth that are wedged in place because of premature tooth loss, severe malocclusion, or major orthodontic concerns. You would probably notice them in your child, or their pediatric dentist would be able to see it during their exam.
When to See a Dentist
Do you have swollen gums around a wisdom tooth? Are you in severe pain, or are your gums sore every time you try to eat? You could have pericoronitis, and you need to have it treated within the next week or two, if not earlier. This type of infection will not go away on its own, even if the symptoms temporarily improve. Request an exam with your dentist or an oral surgeon who specializes in treating wisdom teeth and keep up with good oral hygiene.
Make your inbox smile!
Subscribe