New COVID-19 Symptom: Sore Roof of Mouth

Since the onset of the COVID-19 virus, we’ve been warned repeatedly by epidemiologists and medical professionals to watch for symptoms of illness that mimic anything from the loss of smell and taste to severe respiratory distress. It seems that the novel coronavirus affects people differently, leading to an extensive list of possible side effects.
Most recently, some of those new “red flags” are the possibility of developing a “mouth rash” or sore roof of the mouth as COVID symptoms. Although mouth sores aren’t present in all COVID cases, they are starting to become frequent enough that a sudden onset of a mouth rash should catch your attention.
Mouth Rash | COVID Mouth Sores
Although it might sound surprising to see mouth sores pop up in certain coronavirus cases, it’s fairly common to observe such “mouth rashes” in people with other viral infections (such as chicken pox or hand, foot, and mouth disease.) Being that the oral mucosa is such a highly sensitive tissue, it isn’t unheard of to see viral manifestations in this delicate part of the body. Especially if you’re going to expect to see the possibility of a rash elsewhere on your skin.
Sore Roof Of Mouth COVID Symptoms
Could having sores or ulcers in the roof of your mouth be due to the coronavirus? Evidently so. While the latest research on COVID-19 doesn’t restrict mouth sores to the palate (roof of the mouth,) it may be easier for people to notice this area first. Especially if they’re having difficulty swallowing or someone is peering into their mouth to see what’s going on. If your oral mucosa is lighter in color, you’ll tend to notice the rash even easier. Individuals with extremely dark pigment in their oral tissues will want to look for ruptured membranes or raised/inflamed points, as red patches may be more challenging to make out.
What Do COVID Mouth Sores Look Like?
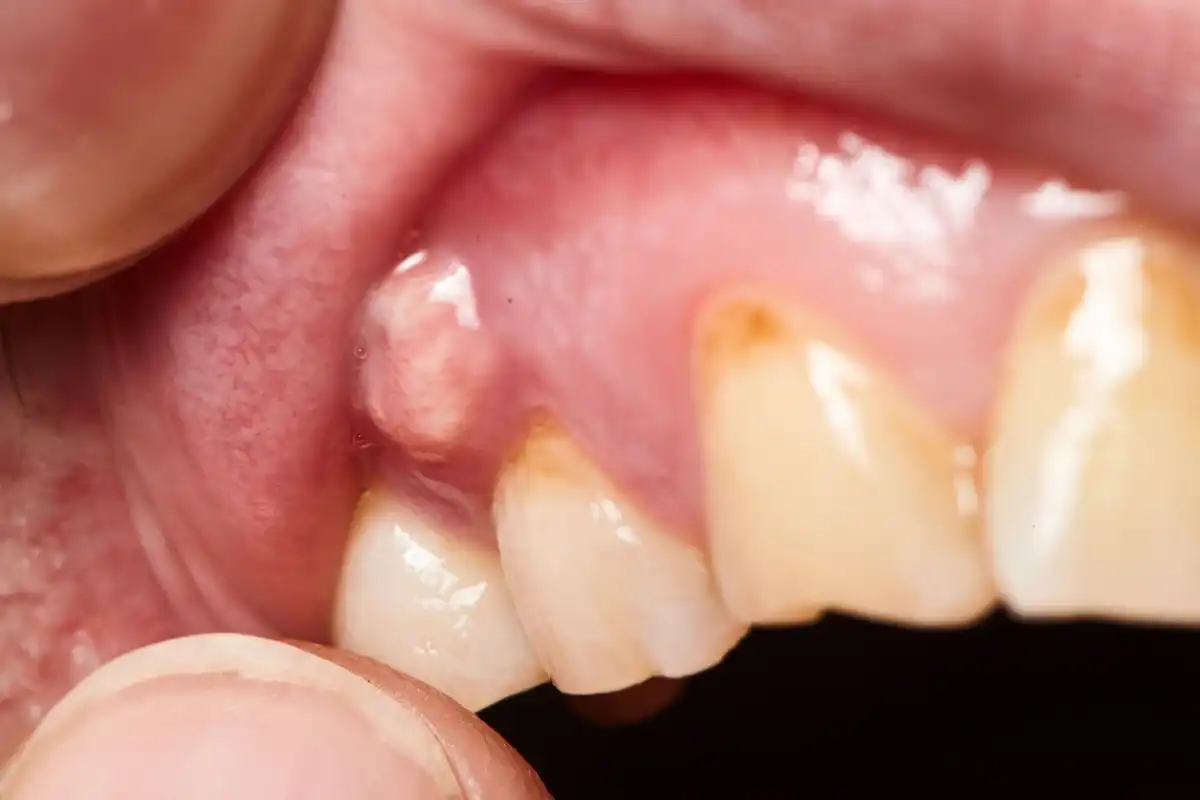
Other people may see multiple red pinprick-sized spots across the roof of their mouth. Or, they might develop significant sores, lumps, or ulcers along the sides and top of their tongue.
Bottom line, a mouth rash will look different than the consistent, smooth coloration you would normally observe inside of your mouth. Affected areas are likely to be extremely tender to the touch, which can make it difficult to speak or swallow.
Medical experts recommend an oral exam be emphasized as part of ICU treatment, due to the extent of oral manifestations as a symptom of COVID-19. When other symptoms may not be evident, linking mouth sores with other common signs of coronavirus may be a good indication of assumed positive infection even if you are still awaiting the formal test results.
Should You Be Concerned About COVID If You Have Mouth Sores?
Although the occasional ulcer or canker sore is nothing to be alarmed about, a sudden plethora of mouth sores or an oral rash should grab your attention. Even though you don’t want to panic, you should be aware that such symptoms could be one of the earliest signs that you’ve been infected by some type of a virus. And in this case, it’s more important than ever to consistently screen yourself for symptoms of COVID-19.
Due to the oral-systemic health connection and a person’s mouth being in such close proximity to their respiratory tract, it’s not surprising to learn of oral sores with COVID-19, given the effect the virus has on the lungs. And as a result, everyday activities like eating or drinking can potentially become extremely challenging. Perform a self-assessment of other COVID-19 symptoms, including regular temperature screenings, and keep your medical doctor updated.
Treatment For COVID Mouth Sores
While there is still a lack of research on the most effective treatments for the novel coronavirus, people with secondary mouth sores have reportedly found treatment with traditional oral anti-viral and anti-fungal medication (to alleviate the severity of their mouth rash.) Again, there is yet to be a proven treatment, so it is more of a trial-and-error of treating the oral symptoms for palliative reasons. In other words, your doctor or dentist may want to give you something for the oral pain caused by the rash until your body heals on its own.
Typically, with a normal ulcer outbreak or mouth rash, we would say to do things like:
- Avoid acidic foods and drinks
- Stick to a soft diet
- Eat cooler foods while avoiding hot ones
- Rinse with lukewarm saltwater to alleviate swelling
- Avoid mouth rinses that contain alcohol
- Regularly rinse your mouth if you’re unable to brush
Until we learn more about COVID-19 and why it causes mouth sores in certain people, all we can do is to treat ulcers or rashes the way we already know how.
How Long Do COVID Mouth Sores Last?
One of the things we’ve repeatedly seen with the coronavirus is how some people bounce back within a couple of weeks like the normal flu, while others are significantly impaired for months at a time.
Again, in the Spanish study related to COVID mouth sores, some people didn’t exhibit oral symptoms until 24 days after other symptoms. This is consistent with the unpredictable timeframe of the length of COVID infections and how that affect people differently.
When To Get Tested
Even if you’re not currently experiencing a fever or any other symptoms of COVID-19, these newly discovered symptoms are significant enough that immediate attention is necessary.
Make your inbox smile!
Subscribe